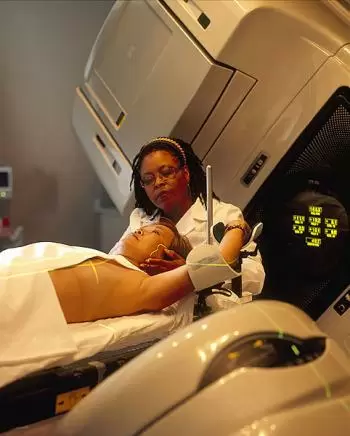
Teletherapy is a medical treatment technique that is part of external radiation therapy used to treat certain diseases, especially cancer. In teletherapy, patients are irradiated with radiation from an external source that is outside their body.
In simpler terms, it is a type of treatment in which X-rays or high-energy particles are used to attack and destroy cancerous or abnormal cells in the body, without the need to insert a radiation source directly into the patient.
The radiation source is in a special device called a linear accelerator, which precisely directs the rays toward the area where the tumor is located.
During treatment, the patient is positioned on a treatment table and immobilized to ensure that the radiation is directed only at the specific area of the body to be treated. X-rays or high-energy particles are applied with the intention of damaging the DNA of cancer cells, impeding their ability to grow and divide, ultimately leading to their destruction.
Teletherapy is a very common and effective treatment for many types of cancer, and is used in both curative and palliative cases. It may also be used along with other treatments such as surgery, chemotherapy, or hormone therapy, depending on the type and stage of the cancer and the specific needs of the patient.
How it is performed?
The teletherapy process begins with a planning phase, where the medical team analyzes the results of the patient's medical examinations and tests to define the exact location and size of the tumor or area to be treated. The radiation dose and the number of sessions necessary for the treatment are also determined.
During the administration of the treatment, the patient is placed in a specific position and is immobilized with special devices to ensure the precision and consistency of the irradiation in each session. These devices may include custom-fit pads, masks, or splints. In addition, reference points are marked on the skin to ensure correct alignment with each session.
The radiation is delivered through specialized medical equipment called a linear accelerator. This device directs X-rays or high-energy particles towards the target area, that is, towards the tumor or the area to be treated. Radiation damages the DNA of cancer cells, preventing their ability to grow and divide, and eventually leading to their destruction.
Risks and side effects
Although teletherapy is a widely used and effective medical treatment, like any medical procedure, it carries certain risks and side effects. Some of the possible risks and side effects associated with teletherapy include:
-
Fatigue: It is common for patients to experience fatigue during and after treatment. Fatigue can vary in intensity and can affect the patient's ability to carry out normal daily activities.
-
Skin Irritation: Radiation can cause redness, itching, and tenderness of the skin in the treated area. These effects are usually temporary and can be managed with creams or lotions prescribed by the medical team.
-
Skin changes: In some cases, the skin in the treated area may become darker or dry, and in rare cases ulcers may appear.
-
Nausea and Digestive Problems: Depending on the area treated, some patients may experience temporary nausea or digestive problems.
-
Hair Loss: If the treated area includes the scalp, temporary hair loss may occur.
-
Problems in nearby areas: Radiation can affect healthy tissue near the treated area, which can cause specific side effects depending on the location of the treatment.
-
Risk of new cancers: Although rare, radiation can increase the risk of developing new cancers in the future.
-
Risk of damage to nearby organs and tissues: Depending on the location of the tumor and the dose of radiation used, there is a risk of damage to nearby organs or tissues.
It is important that patients discuss any concerns or symptoms they may experience during treatment with their medical team.
Techniques and types of teletherapy
Teletherapy, or external radiation therapy, can vary depending on the source of radiation used and the techniques used. Here are some common types of teletherapy:
-
X-ray teletherapy: It is the most common type of teletherapy, where high-energy X-rays generated by a linear accelerator are used. X-rays are directed toward the targeted area to kill cancer cells.
-
Electron Teletherapy: Instead of using X-rays, accelerated electrons are used in a linear accelerator. Electron irradiation is used to treat tumors that are superficial or located close to the skin, since electrons have less penetration into tissue compared to X-rays.
-
Proton Teletherapy: In this approach, positively charged protons are used instead of X-rays. The protons release most of their energy at a specific point deep, reducing the dose to tissues near the target area. Proton therapy is used to treat tumors near critical organs or in sensitive areas.